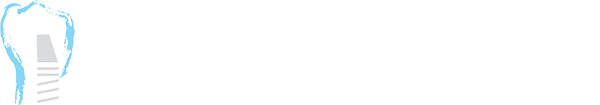Most adults with gum disease don’t feel pain until damage is already underway. That’s why understanding when to see a periodontist instead of a general dentist can make a real difference in preventing bone loss and tooth loss. While routine cleanings and exams are essential, certain symptoms—like persistent bleeding gums, gum recession, or a gum abscess—may require specialist care. Knowing when to seek advanced periodontal evaluation can help protect the long-term health of your teeth and supporting bone.
When to See a Periodontist vs. a General Dentist: Start Here
A general dentist is your primary dental provider for prevention and everyday problems. Think exams, prophylaxis visits, dental cleaning appointments, dental X-rays, radiographs, fillings, crowns, night guards for clenching, and first-line gum inflammation care.
In addition, general dentists monitor plaque and calculus (tartar) buildup, coach home care, and spot early gingivitis before it progresses into periodontitis. When findings suggest deeper periodontal pockets, persistent bleeding on probing, or clinical attachment level changes, they typically make a referral for specialty care.
A periodontist is a dental specialist with advanced training in periodontics, focusing on the periodontium — the gums, the periodontal ligament that anchors the teeth, and the alveolar bone that supports them. They diagnose and treat periodontitis, manage pocket depth, rebuild lost attachment, and preserve the supporting bone structure.
This distinction matters because periodontitis is not just sore gums — it is a progressive bone-loss disease. For that reason, understanding when to see a periodontist can make a measurable difference. Earlier specialist care can slow clinical attachment level decline, reduce pocket depth, and lower the risk of tooth mobility, shifting teeth, and long-term bite changes.
The American Academy of Periodontology outlines how specialists diagnose and manage gum disease, including advanced periodontitis and implant-related complications.
Training and Focus Areas (Periodontics as a Specialty)
After dental school, periodontists complete advanced specialty training focused on gum disease, infection control, bone regeneration, and surgical precision. That extra training becomes especially important in cases involving furcation involvement, deep periodontal pockets, or advanced periodontitis.
They also frequently use CBCT imaging when evaluating implant placement, sinus lift procedures, or complex bone defects. This level of diagnostic precision allows for guided tissue regeneration and predictable bone grafting outcomes.
There is overlap, of course. Mild gingivitis and routine dental cleaning visits may still be managed by a general dentist. However, when pocket depth remains elevated or bleeding on probing persists, specialist evaluation becomes more appropriate.
Symptoms That Mean You Should Book a Periodontist Consultation
Bleeding gums that continue despite improved brushing technique and flossing deserve further evaluation. While occasional bleeding can occur, persistent gum inflammation often signals deeper periodontal probing findings. If you’re unsure when to see a periodontist, bleeding that does not improve after routine dental cleanings is often a clear sign that a specialist evaluation may be necessary.
Gum recession is another common indicator. If your teeth appear longer, roots become exposed, or you develop root sensitivity, a periodontist can identify whether inflammation, trauma, malocclusion, or thin soft tissue is causing the problem.
Persistent bad breath (halitosis), a bad taste, or infection that returns after dental cleaning may indicate bacteria living in deep periodontal pockets.
Loose teeth, tooth mobility, or bite changes are late-stage warning signs. In many cases, these symptoms correlate with attachment loss and measurable bone loss visible on radiographs.
Red-Flag Signs That Should Not Wait
A gum abscess or periodontal abscess often presents as pus at the gumline, localized swelling, and pain on chewing. This is not something to monitor at home. It typically requires immediate evaluation and may involve local antimicrobial therapy in addition to mechanical cleaning.
If swelling spreads, fever develops, or swallowing becomes uncomfortable, seek urgent care the same day.
Clinical Findings That Often Trigger Referral
General dentists frequently refer when:
- Pocket depth remains 5mm or greater
- Bleeding on probing persists
- Clinical attachment level worsens
- Radiographs show progressive alveolar bone loss
- Furcation involvement is detected
- Tooth mobility increases
These findings indicate disease beyond simple gingivitis. These findings indicate disease beyond simple gingivitis. When you’re unsure when to see a periodontist, measurements like persistent deep pockets, attachment loss, or visible bone loss on radiographs are strong clinical signals that specialist care is appropriate.
Higher-Risk Patients Who Benefit From Specialist Oversight
Certain risk factors increase disease progression:
- Smoking and vaping
- Diabetes
- Pregnancy gingivitis
- Family history of early tooth loss
- Poorly controlled plaque and tartar accumulation
Because these factors impair healing, a periodontist may recommend more frequent periodontal maintenance visits than standard prophylaxis intervals.
Procedures That Usually Belong With a Periodontist
Scaling and root planing (deep cleaning) removes calculus and bacterial deposits below the gumline. In more advanced cases, local antimicrobial therapy may be used in stubborn areas.
When non-surgical care is insufficient, periodontal surgery may be recommended. Learn more about the signs gum surgery may be necessary. Options include:
- Flap surgery
- Pocket reduction surgery
- Soft tissue graft
- Connective tissue graft
- Free gingival graft
- Root coverage procedures
- Bone grafting
- Guided tissue regeneration
- Bone regeneration
In advanced cases, laser periodontal therapy may be considered, although it is not necessary for every patient. If you’re unsure when to see a periodontist, needing surgical procedures, grafting, or bone regeneration is typically a clear indication that specialist treatment is appropriate.
Dental Implants and Bone Support
Periodontists also handle implant consultations and implant placement, especially when patients need bone grafting or a sinus lift to create adequate bone support.
They evaluate risk factors for peri-implantitis, which can compromise implant stability. Proper planning protects long-term implant survival and reduces complications.
If you’re exploring options for replacing a missing tooth with a dental implant, understanding long-term bone support is essential.
What to Expect at a Periodontist Visit
Your visit typically includes:
- Full periodontal probing
- Measurement of clinical attachment level
- Tooth mobility grading
- Evaluation of furcation involvement
- Radiographic bone assessment
- Discussion of treatment plan and insurance coverage
Many periodontists accept self-referral, although some insurance plans require formal referral documentation.
Home Care and Long-Term Stability
Treatment success depends on consistent home care. Proper brushing technique, flossing, interdental brushes, or a water flosser may be recommended depending on pocket depth and anatomy.
Chlorhexidine rinses or local antimicrobial therapy may be used short-term in select cases.
Periodontal maintenance visits are typically scheduled every 3–4 months, not twice per year. This is because periodontal pockets can repopulate with bacteria more quickly in susceptible patients.
Common Mistakes That Delay the Right Care
Waiting for pain is the biggest mistake. Periodontitis often progresses quietly.
Ignoring persistent bleeding gums, halitosis, swollen gums, or recurring infection allows attachment loss and alveolar bone damage to continue.
Stopping periodontal maintenance once symptoms improve also increases relapse risk.
FAQ (Optimized for Yoast)
Can I go straight to a periodontist if I’m unsure when to see a periodontist? Yes. Many specialists accept self-referral, especially for gum recession, gum abscess, dental implants, or suspected periodontitis.
What is clinical attachment level?
Clinical attachment level measures how much support a tooth has lost from the periodontium. It is one of the most important indicators of disease progression.
Is deep cleaning the same as regular dental cleaning?
No. Scaling and root planing treats periodontal pockets below the gumline. Prophylaxis treats plaque and tartar above the gumline.
When is gum surgery necessary?
Gum surgery is recommended when non-surgical therapy cannot sufficiently reduce pocket depth or stop bone loss.
If you’re unsure when to see a periodontist, scheduling an evaluation with a Houston periodontal specialist can provide clarity and protect your long-term oral health.