A loose tooth in adults is rarely “just one of those things.” Adult tooth mobility is usually a warning sign that the support system around a permanent tooth — the gums, periodontal ligament, and bone — is breaking down or has been injured.
A loose tooth in adults should never be ignored. According to Cleveland Clinic, permanent teeth should not move, and mobility is usually a sign of underlying gum, bone, or structural damage.
The good news is that many loose teeth can be saved when the cause is found early and treated correctly. The bad news is that waiting often turns a fixable problem into a non-restorable tooth.
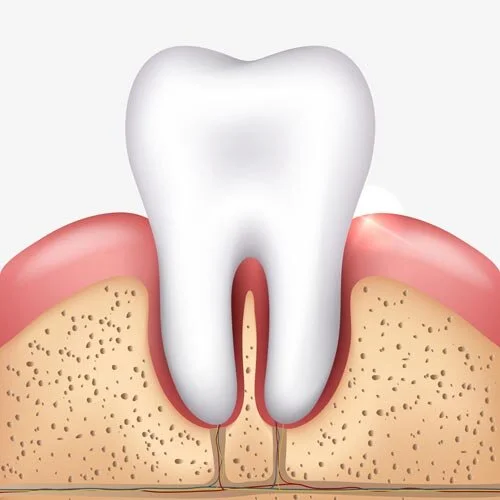
A “loose” tooth in adults can mean two very different problems. One is loss of gum and bone support, often from periodontal disease, and the other is structural damage like a cracked tooth, root fracture, or trauma-related injury.
Inflammation and bite overload can sometimes reduce mobility once the tissues calm down and clinicians control the forces. A vertical root fracture or severe alveolar bone loss makes mobility far harder to reverse.
Time matters because the causes tend to progress. Gingivitis can advance to periodontitis, periodontal pockets can deepen, and attachment loss can accelerate, especially if smoking or diabetes is in the picture.
Dentists usually weigh a few decision factors to estimate “savable vs. not savable.” The big ones are how much bone remains around the root, whether there’s active infection, whether the root is intact, and whether the tooth has enough structure above and below the gumline to support restoration.
Mild to moderate mobility with swollen gums and bleeding gums often improves when treatment reduces inflammation and patients control plaque. If periodontal ligament irritation mainly causes the looseness, the tooth often tightens after deep cleaning, bite changes, and healing time.
A tooth may also be salvageable when there is no vertical root fracture and pain or swelling improves with infection control.
For example, a pulp infection can create a dental abscess near the root tip. It can sometimes mimic mobility. Root canal therapy may resolve it if periodontal support is still adequate.
Severe mobility combined with advanced periodontitis usually signals major attachment loss and alveolar bone loss.
If the bone support is reduced to the point that the tooth moves in multiple directions, chewing may feel unstable. At that stage, saving it becomes unpredictable in a loose tooth in adults.
Certain findings often push a tooth into “poor prognosis” territory in cases of a loose tooth in adults.
These include furcation involvement in molars, a vertical root fracture, non-restorable decay below the gumline, or repeated abscesses that return despite treatment.
Periodontal disease is the most common driver of adult tooth mobility. As gum tissue detaches and bone resorbs, the tooth loses the support that normally keeps it firm.
Dental trauma is another major cause, especially after a sports injury, fall, or blow to the face.
Trauma can damage the periodontal ligament. It can loosen the tooth in its socket. It can also cause a cracked tooth or root fracture that changes the long-term outlook.
Bite-related issues can also loosen teeth over time.
Bruxism, occlusal trauma, and a “high” filling or crown contact can concentrate force on one tooth. Over time, the tissues around it become inflamed and the tooth starts to move.
Systemic and lifestyle factors often make the same dental problem worse.
Smoking, poorly controlled diabetes, and conditions that affect bone metabolism such as osteoporosis can reduce healing capacity and increase periodontal breakdown.
Periodontitis usually starts with plaque and calculus accumulating along the gumline.
The body responds with inflammation. The gums can become tender, swollen, and prone to bleeding in cases of a loose tooth in adults.
As the disease progresses, a periodontal pocket forms and deepens. It traps more bacteria where brushing cannot reach.
Over time, attachment loss and alveolar bone loss reduce support. The tooth begins to feel loose, especially when biting. This is a common cause of a loose tooth in adults.
Gum recession is common in this process.
It is not just a cosmetic issue. It often reflects underlying bone loss and root exposure that increases tooth sensitivity in a loose tooth in adults.
If you want a deeper look at how gum problems lead to tooth instability and eventual loss, see this explanation of how advanced gum disease can lead to losing teeth: https://drfriedbergandassociates.com/gum-disease-tooth-loss/
Not all mobility is periodontal. A pulp infection inside the tooth can spread out the root tip, causing a dental abscess and localized bone changes that make the tooth feel tender, “taller,” or slightly mobile.
When the tooth is structurally sound and the surrounding periodontal support is reasonable, endodontic treatment can help. Root canal therapy removes infected tissue, disinfects the canal system, and allows the bone around the root to heal over time.
This is why dentists often test both the gums and the nerve of the tooth. A tooth can have both periodontitis and endodontic infection, and the treatment plan changes when both problems exist.
Diabetes increases periodontal risk because elevated blood sugar can impair immune response and slow healing. People with diabetes also tend to have more severe gum inflammation when plaque control slips.
Smoking and vaping reduce blood flow to the gums and make periodontal therapy less predictable. They also mask bleeding, so gum disease can look “quiet” while bone loss continues.
Osteoporosis does not automatically cause loose teeth, but lower bone density and some medications can influence oral health. Your dentist may ask about bone medications, fracture history, and recent medical changes because they can affect surgery planning and healing.
Treat an adult loose tooth as urgent, not as something to monitor for weeks. Call a dental office promptly and describe how loose it feels, whether it happened suddenly, and whether there is tooth pain, swelling, or a bite change related to a loose tooth in adults.
Protect the tooth from extra force. Chew on the other side, stick to soft foods, and avoid biting into hard items like crusty bread, nuts, ice, or jerky.
Control inflammation safely while you wait. Brush gently along the gumline, floss carefully if it does not worsen pain, and use warm salt-water rinses to soothe irritated tissue.
Over-the-counter pain relief can help if you can take it safely. Follow the label and consider calling your pharmacist or physician if you are on blood thinners or have medical restrictions.
If dental trauma occurred, write down the timing and symptoms. Note whether something hit the tooth, whether it moved immediately, and whether you now have tooth sensitivity to cold or pressure, because that information helps the dental team triage the risk of ligament injury or pulp infection.
Do not wiggle the tooth “to check it.” Repeated movement can worsen periodontal ligament injury and can disrupt early healing.
Do not attempt DIY splinting, gluing, or “tightening” the tooth. Household adhesives are not safe in the mouth, and incorrect splinting can trap plaque and accelerate inflammation.
Do not ignore pus, facial swelling, fever, or worsening pain. Those signs can indicate a spreading infection that needs urgent evaluation.
Same-day evaluation is appropriate after trauma, rapidly increasing mobility, facial swelling, or a sudden bite change where the teeth no longer fit together normally. Those patterns can signal ligament damage, fracture, or an active dental abscess.
Seek immediate care if you have trouble swallowing, feel systemically ill, or swelling is spreading. This crosses into dental emergency territory, especially when infection may be moving beyond the tooth.
Saving a loose tooth starts with a precise diagnosis, not a guess. Dentists typically use periodontal probing to measure pocket depths, grade mobility, check the bite, and take dental X-rays, sometimes adding CBCT imaging when they suspect a root fracture or complex infection.
Treatment usually targets the cause first. Stabilizing a tooth without controlling periodontal disease, infection, or occlusal trauma often fails because the same forces and bacteria keep damaging the support.
After clinicians control the cause, stabilization can help the tooth function while tissues heal. Options include splinting with a dental splint, occlusal adjustment, a night guard for bruxism, and restorative changes such as replacing a poorly fitting dental crown that traps plaque or creates a high contact.
When saving the tooth becomes unpredictable, replacement planning should happen early. Discussing a dental implant, dental bridge, or partial denture ahead of time helps protect function and can preserve bone when the timing is right.
Scaling and root planing, often called deep cleaning, removes plaque and hardened calculus from below the gumline. Reducing bacterial load can shrink swollen gums, decrease pocket depth, and improve comfort, which can reduce mobility when inflammation drives the problem.
For more advanced periodontitis, clinicians may recommend periodontal surgery to access deep deposits, reshape tissues, or manage defects. In select cases, clinicians use bone graft procedures to support regeneration, although results depend on defect type, hygiene, and risk factors like smoking and diabetes.
Long-term success depends on periodontal maintenance. Dentists commonly schedule cleanings at 3 to 4 month intervals for patients with a history of periodontal pockets, because relapse happens quickly when biofilm control slips.
Root canal therapy is used when pulp infection is causing pain, swelling, or an abscess, and the tooth is restorable. The goal is to eliminate infection inside the tooth so the bone around the root can heal in cases of a loose tooth in adults.
If conventional treatment is not enough, an apicoectomy may be considered in select cases. This involves removing infected tissue at the root tip and sealing the end, usually when anatomy or prior work prevents full disinfection from inside the tooth.
Endodontic treatment cannot compensate for severe periodontal support loss. If the tooth is loose mainly because of extensive attachment loss, the plan must address the gums and bone first.
Splinting connects a loose tooth to neighboring teeth so biting forces distribute during healing. A dental splint may serve as a temporary solution after dental trauma or as a semi-permanent option when periodontal support decreases but remains adequate for function.
Bite management matters because force can keep a tooth mobile even after clinicians control the infection. An occlusal adjustment or bite adjustment can remove a high contact, and a night guard can reduce damage from bruxism that occurs during sleep.
If a restoration contributes to the problem, fixing it can become the turning point. Replacing an over-contoured crown, correcting a high filling, or addressing a cracked tooth can reduce occlusal trauma and plaque retention.
Extraction is often recommended when a vertical root fracture is confirmed. It is also recommended when decay extends too far below the gumline. Periodontal support loss can also make the tooth non-restorable.
Keeping a failing tooth “a little longer” can sometimes accelerate bone loss and complicate replacement.
If removal is needed, talk through replacement options early.
A dental implant is often considered because it can replace the root and help preserve bone. A dental bridge or partial denture may be appropriate depending on bite, budget, and adjacent teeth.
For patients weighing implants, these two resources explain the reasoning and timing in plain terms: read about reasons to choose an implant for a missing tooth (https://drfriedbergandassociates.com/why-should-i-consider-a-dental-implant-to-replace-my-missing-tooth/) and why implants are often discussed soon after extraction (https://drfriedbergandassociates.com/why-would-i-get-dental-implants-after-a-tooth-extraction/).
If you need details on the extraction process itself, this overview of surgical removal and aftercare is helpful: https://drfriedbergandassociates.com/oral-surgery/tooth-extractions/
A common scenario is gum-related mobility that improves after periodontal therapy.
A patient with bleeding gums, a 5 to 6 mm periodontal pocket, and mild mobility may feel the tooth firm up after scaling and root planing. This is followed by consistent periodontal maintenance for a loose tooth in adults.
Trauma is another example.
After a sports injury, a tooth may be mobile because the ligament is bruised. Splinting for a few weeks plus a soft diet can allow the tooth to stabilize if there is no root fracture.
Endodontic cases can look dramatic but respond well.
A tooth with tooth pain to biting and a localized abscess on X-ray may calm down after root canal therapy. This happens when the tooth structure and gum support are still strong.
Costs vary because the “loose tooth” is a symptom, not a diagnosis.
The final plan may include imaging, deep cleaning, splinting, root canal therapy, a dental crown, periodontal surgery, bone grafting, or tooth extraction and replacement.
Mistakes tend to cluster around delay and force.
Waiting months, chewing hard foods on the loose tooth, skipping maintenance visits after gum treatment, and ignoring bruxism are some of the quickest ways to turn a manageable problem into a tooth-loss situation.
Severity and cause drive the plan. Periodontal disease may require deep cleaning and ongoing maintenance, while an endodontic problem may require root canal therapy and a crown, and trauma may need splinting plus follow-up testing.
Geography and provider type also affect cost. A periodontist or endodontist, advanced imaging like CBCT, and complex restorations can raise the total, so diagnosis comes first and estimates come second.
If gum disease caused the mobility, prevention is mostly about consistency. Daily plaque removal at the gumline, interdental cleaning, and periodontal maintenance at the interval your dentist recommends reduce the chance that periodontal pockets deepen again.
If bite forces contributed, address them directly. Wear the night guard as prescribed, follow through with occlusal adjustment when recommended, and replace failing restorations that trap plaque or create high contacts.
Sometimes, yes. If the looseness is from inflammation (gingivitis or early periodontitis) or from bite trauma, treating the cause with scaling and root planing, splinting, and bite adjustment can reduce mobility.
It rarely improves on its own, and “testing it” by wiggling usually makes it worse.
A tooth is often not savable with a confirmed vertical root fracture, non-restorable decay below the gumline, or severe periodontal bone loss that leaves inadequate support. Repeated abscesses and advanced furcation involvement also tend to lower predictability.
Your dentist will combine mobility findings, periodontal probing numbers, and dental X-rays to make that call.
It depends on the cause and how many steps are needed. Some cases involve deep cleaning and maintenance, while others require splinting, root canal therapy, a dental crown, periodontal surgery, or extraction and replacement.
A dentist has to diagnose first before any accurate estimate is possible.
Yes. Delaying care can allow infection or alveolar bone loss to progress, reducing the chance of saving the tooth and sometimes affecting neighboring teeth.
If there is swelling, pus, fever, or facial swelling, treat it as urgent rather than waiting for it to “settle down.”