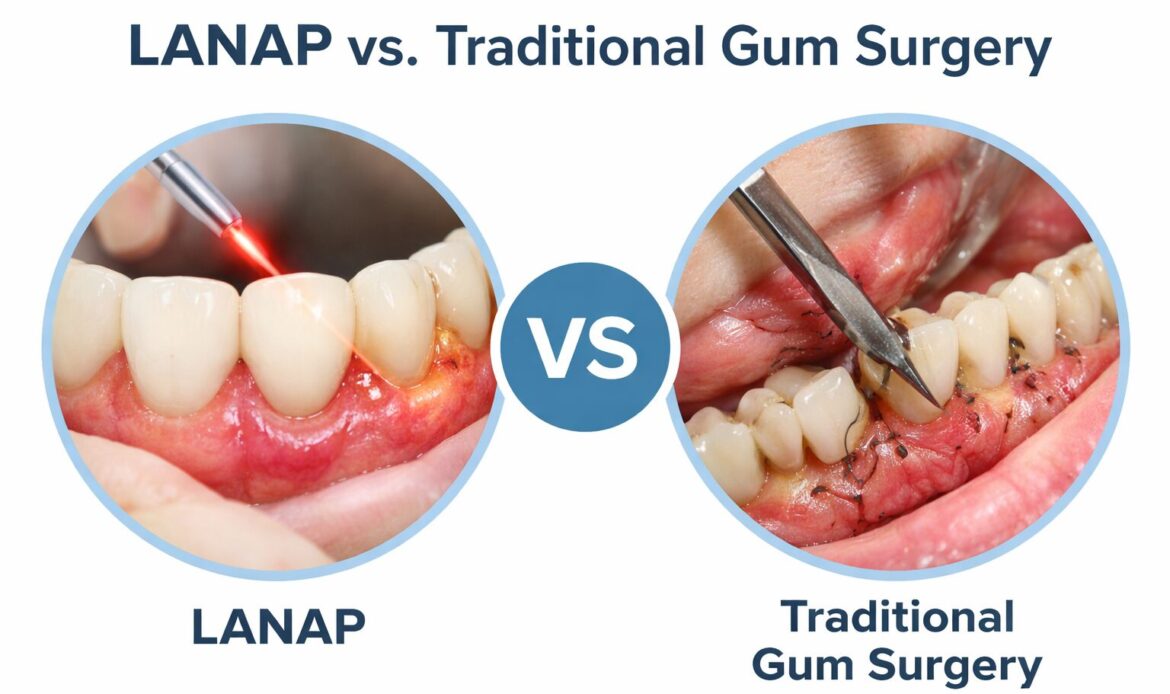
When comparing LANAP vs traditional gum surgery, the word “better” usually comes down to two numbers your periodontist measures. These include periodontal pocket depth and clinical attachment level. If a procedure helps control bacteria and biofilm while improving cleanability, it has a real chance of protecting bone support. It may also lower tooth loss risk.
LANAP laser gum surgery can be a strong option for the right case. This is especially true when you want a minimally invasive approach and a smoother recovery time. Traditional gum surgery still matters because some periodontitis patterns need direct access, bone recontouring, or regeneration steps. Lasers cannot replace those techniques in certain cases.
What Problem Both Procedures Treat: Periodontal Disease
Periodontal disease is an infection-driven inflammation of the gums and supporting structures. It deepens gum pockets and threatens the bone that holds teeth in place. According to the National Institute of Dental and Craniofacial Research, untreated gum disease can progress and lead to bone loss and eventual tooth instability.
Common triggers include plaque that matures into a sticky biofilm. Tartar or calculus can trap bacteria. Risk factors include smoking, diabetes, genetics, and inconsistent home care. Once tartar forms below the gumline, brushing alone cannot remove it.
The goals of surgery are practical and measurable. They include reducing periodontal pocket depth, improving infection control, stabilizing attachment, and making daily cleaning possible again. The end goal is long-term protection. That means keeping inflammation low and maintenance realistic.
Signs You May Need Surgical Periodontal Treatment
Bleeding that does not stop, persistent bad breath, gum recession, and tooth sensitivity from root exposure are common red flags. Pus, pain when chewing, and tooth mobility can signal more advanced gum disease — and may lead to a discussion about LANAP vs gum surgery as treatment options.
Another common scenario is deep pocket depths that remain after scaling and root planing, with ongoing inflammation at recheck. If pockets stay deep, bacteria repopulate quickly and the cycle continues.
When Non-Surgical Care Isn’t Enough
Scaling and root planing can work well for mild cases, especially when pockets are shallow and anatomy is straightforward. It becomes less predictable when pockets are deep, furcations are involved, or calculus is tenacious and hard to access.
Surgery is typically considered when pockets remain deep after root debridement and the risk of continued bone loss stays high. If you are unsure where you fall on that spectrum, this overview on when surgical treatment becomes the next step lays out common decision points.
How Traditional Gum Surgery Works (Flap Surgery and Osseous Surgery)
Traditional gum surgery often refers to flap surgery. It may be combined with osseous surgery or pocket reduction surgery. The point is simple: reflect a periodontal flap so the periodontist can see and clean roots and bone directly. This direct access is one of the key differences when comparing LANAP vs gum surgery.
A typical sequence includes local anesthesia. The clinician then gently lifts the gum tissue away from the tooth. Next, inflamed tissue is removed, followed by debridement and root planing. Bone reshaping may also be performed with recontouring if the defect pattern calls for it.
Afterward, the clinician repositions the gums and secures them with sutures. Many offices also offer sedation dentistry for anxious patients or longer appointments, depending on medical history and the treatment plan.
Expect swelling, some bleeding, and post-op discomfort for several days. You will also follow a specific hygiene and diet plan while healing progresses. The periodontist uses follow-up visits to check healing, remove sutures if needed, and confirm pocket reduction.
Traditional surgery works best when heavy calculus is present. It also helps when defects require precise access or when significant osseous changes are needed. If the bone architecture requires reshaping to create maintainable contours, open access can be the most efficient route.
Traditional Surgery Pros and Tradeoffs
Traditional surgery offers direct visibility and access, which can be valuable in advanced cases. It also allows a periodontist to address complex anatomy and aim for predictable pocket reduction when disease is severe.
The tradeoffs are usually felt in recovery time. Patients often report more swelling, more bleeding, and more post-op discomfort than minimally invasive approaches, plus a higher chance of gum recession and tooth sensitivity from additional root exposure.
Common Add-Ons in Conventional Periodontal Surgery
Some defects benefit from regeneration techniques designed to rebuild lost support. Bone grafting and guided tissue regeneration may be recommended when defect shape and stability make new bone fill more likely.
Recession may require a gingival graft or connective tissue graft, either at the same time or as a staged procedure. If aesthetics or sensitivity are major concerns, you may want to read about periodontal plastic surgery options offered in Houston and how grafting decisions are typically made.
How LANAP Works (Laser-Assisted New Attachment Procedure)
Unlike traditional flap approaches discussed in LANAP vs gum surgery comparisons, this procedure stands for Laser-Assisted New Attachment Procedure and is not just “any laser.” The treatment follows a specific protocol performed with an Nd:YAG laser, commonly the PerioLase MVP-7, using defined steps and settings aimed at targeting diseased tissue and bacteria while preserving healthy tissue.
Treatment typically begins with a first laser pass to remove diseased pocket lining and reduce bacterial load. Ultrasonic scaling and root debridement follow, often using an ultrasonic scaler to disrupt biofilm and remove calculus from the root surface.
The clinician then performs a second laser pass to help create a stable fibrin clot at the gumline, which acts like a biological seal. The periodontist may also adjust the bite when trauma from occlusion or clenching contributes to inflammation or mobility.
LANAP is often positioned as a minimally invasive option for mild to moderate periodontitis, but case selection matters. For a step-by-step explanation of what patients usually experience, see this overview of the laser-based protocol and what it involves.
Potential Benefits Patients Notice With LANAP
Many patients notice less bleeding and swelling, and often fewer or no sutures. That usually translates to a faster return to normal activities and a more comfortable first week.
Post-op discomfort is often lower than with flap surgery, though it is not “no recovery.” You still have healing time, diet guidelines, and a maintenance plan to protect results.
Limits and Candidacy Considerations
LANAP is not ideal for every case, especially when severe bone loss patterns require extensive osseous recontouring. Some localized defects also benefit from direct access or combined approaches, depending on anatomy and goals.
Outcomes depend heavily on clinician training, laser settings, and how well clinicians maintain infection control afterward. Home care and periodontal maintenance are not optional, because bacteria and biofilm can re-establish quickly in high-risk patients.
LANAP vs Traditional Gum Surgery: What “Better” Means in Real Life
If your main concern is pain and downtime, LANAP often wins on patient experience because it is less invasive. If your main concern is access for advanced defects, traditional gum surgery may be the more predictable tool.
Recession risk is another real-life factor. Flap reflection and suturing can increase the chance of gum recession and tooth sensitivity, while laser protocols may preserve more tissue in some cases, although outcomes vary by anatomy and inflammation level.
Discuss pocket reduction goals in numbers, not generalities. Ask what pocket depths you can expect to improve, how the clinician will track clinical attachment level, and what maintenance interval you will follow once inflammation comes under control.
Long-term habits usually determine results after surgery, not the procedure itself. Periodontal maintenance, daily plaque control, and addressing smoking or diabetes management often make the difference between stability and relapse.
Cost and insurance coverage can also drive the decision. In some markets, practices may price LANAP higher, and insurance plans vary coverage based on coding and documentation, so verify benefits before committing.
Side-by-Side Comparison Checklist
- Invasiveness: LANAP uses a dental laser within the pocket, while traditional surgery reflects a periodontal flap and often uses sutures.
- Recovery: LANAP often has less swelling and bleeding, while flap surgery may involve a longer recovery time and more diet restrictions.
- Follow-ups: both require re-evaluation and a periodontal maintenance schedule, but traditional surgery may require suture removal and more early post-op visits.
- Results focus: LANAP aims to reduce infection and support new attachment, while traditional approaches can combine cleaning with bone recontouring or regeneration steps when needed.
Questions to Ask a Periodontist Before Choosing
If you are weighing LANAP vs gum surgery, ask for your pocket depths by tooth, your bone loss pattern, and a prognosis tooth-by-tooth. If you hear “moderate” or “severe,” ask what that means in millimeters and what the risk is for attachment loss progression.
Ask what outcomes are realistic for pocket reduction, recession risk, tooth stability, and the maintenance interval. If you are weighing value, this breakdown on whether the investment tends to pencil out for your situation can help frame the decision.
Examples and Common Mistakes That Affect Results
Two patients can get the same procedure and have very different outcomes because periodontitis is a bacterial disease with behavioral and medical drivers. The tool matters, but infection control and consistency matter more.
Clinicians sometimes use antibiotics as an adjunct, but they do not replace mechanical removal of plaque, calculus, and biofilm. If home care and recall fall apart, inflammation returns and pockets deepen again.
The best results usually come from collaboration: clinician skill, smart case selection, and a patient who follows instructions and keeps periodontal maintenance appointments. That includes daily interdental cleaning, and this explanation of why flossing is not optional for gum stability connects the dots between technique and long-term gum health.
Example Scenarios (What Tends to Be a Good Fit)
Mild to moderate periodontitis with persistent pockets after scaling and root planing can be a LANAP consideration. This is especially true when the goal is reducing inflammation with minimal tissue disruption. Patients in this category often have 5 to 7 mm pockets in several areas. They also want less downtime when comparing LANAP vs gum surgery.
Generalized advanced disease with widespread deep pockets, heavy calculus, and mobility may lean traditional. This is particularly true if the periodontist needs access to fully debride roots and correct bony architecture. In some treatment plans, clinicians use a combined approach. Different areas may receive different methods depending on the LANAP vs gum surgery decision.
Localized deep defects sometimes benefit from traditional access plus guided tissue regeneration or bone grafting when defect shape supports regeneration. A laser may still be part of the plan, but it is not always the primary driver of the result.
Mistakes to Avoid After Either Procedure
Skipping periodontal maintenance visits is the fastest way to lose ground, because plaque matures into biofilm and calculus returns. Most stable patients need a 3 to 4 month recall at first, not a standard 6 month schedule.
Smoking or vaping during healing increases complication risk and slows tissue response. Aggressive brushing too soon can disrupt healing tissue. Ignoring bite issues or clenching can also keep inflammation active, even after the pockets improve.
FAQ
Is LANAP better than gum surgery?
It can be, for the right candidate. LANAP is often less invasive with an easier recovery, but traditional gum surgery may be the better choice for severe periodontitis or when bone reshaping and direct access become necessary.
Is laser gum surgery better than traditional?
“Better” depends on your pocket depths, bone loss pattern, and goals. Laser gum surgery may reduce bleeding and downtime for many patients, while traditional surgery can offer more predictable access for advanced cases and complex defects.
Is laser surgery better than regular surgery?
Not universally. A dental laser is a tool, and outcomes still depend on diagnosis, clinician skill, and periodontal maintenance, plus factors like smoking and diabetes control.
What are the downsides of LANAP?
Potential downsides include higher cost in some practices, variable insurance coverage, and the fact that not all severe or complex cases are ideal for the LANAP Protocol. Results also rely heavily on case selection, home care, and ongoing maintenance to keep bacteria and inflammation under control.