If your dentist told you that you need a dental implant, one of your first questions may be whether your jawbone is strong enough to support it. When patients ask about Bone Grafting for Dental Implants: When Is It Necessary?, they usually want to understand whether extra treatment is truly needed or simply optional. This guide explains why bone matters, when dentists recommend grafting, how dentists evaluate the site, and what recovery usually involves.
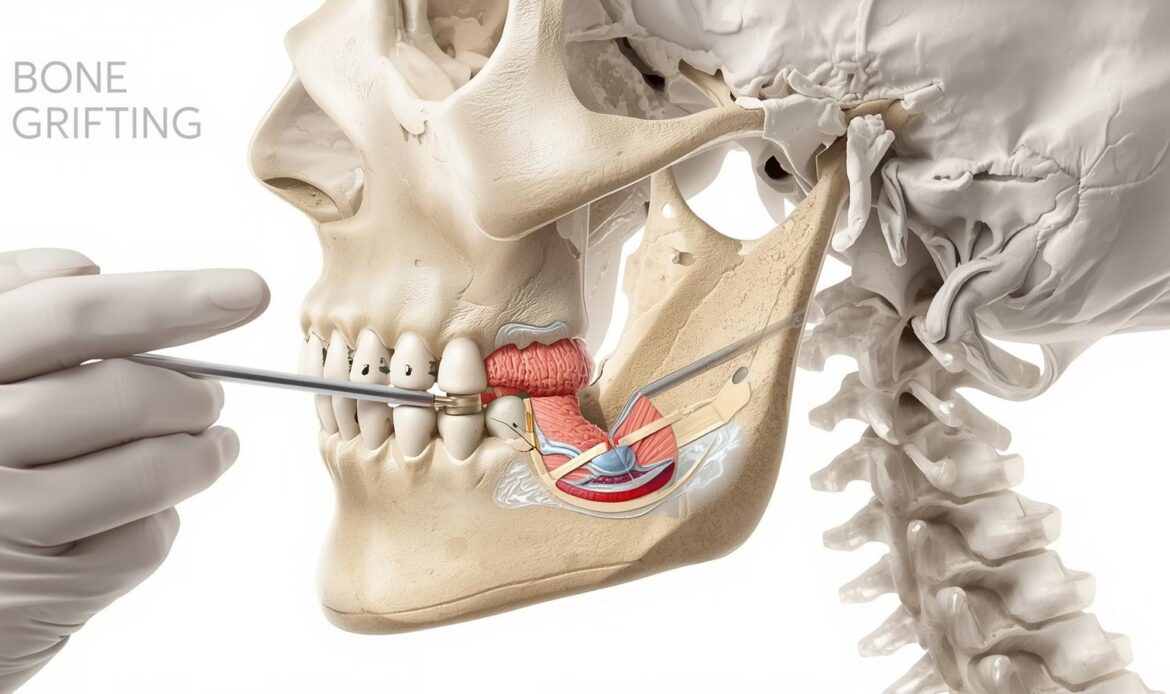
Why Bone Grafting for Dental Implants May Be Necessary
Dental implants depend on the jawbone for long-term stability. For implant success, the site needs enough bone height, bone width, bone volume, and bone density to support osseointegration.
Osseointegration is the process where the implant fuses with surrounding bone. If the jawbone is too thin, too short, or too weak, implant placement becomes less predictable.
Bone loss often begins after tooth loss because the bone no longer receives stimulation from the natural tooth root. This process, called bone resorption, can gradually shrink the ridge and leave too little support for a future implant.
The longer a tooth is missing, the more likely it is that bone volume will decrease. Denture wear, gum disease, periodontal disease, infection, and trauma can accelerate that loss.
Not every implant patient needs a dental bone graft. Many people still have enough native bone for safe treatment, but careful evaluation is essential before deciding.
Bone grafting for dental implants rebuilds or preserves lost bone in the jaw. Patients who want to understand how a dental bone graft procedure works can review additional medical guidance from Cleveland Clinic.
A graft can also improve support around a future implant area where the ridge has collapsed. In some cases, dentists perform socket preservation or ridge preservation immediately after extraction to reduce future shrinkage.
Bone loss happens for several common reasons. These include long delays after extraction, advanced gum disease, untreated infection, failed dental implants, and injuries that damage the supporting bone.
The key point is simple: implants need a healthy foundation. A dentist, periodontist, or oral surgeon must confirm that the bone can support both function and esthetic outcome before moving forward.
When Bone Grafting for Dental Implants Is Necessary
Dentists usually recommend a bone graft when there is not enough healthy bone to place an implant safely and securely. The most common reasons are inadequate bone height, limited bone width, poor bone quality, or anatomical limitations near important structures.
This decision is not based on guesswork. It comes from a clinical exam, digital imaging, and the goals of the treatment plan.
Some patients need bone grafting at the time of tooth extraction. Others may not learn they need it until months or years later, after bone resorption has already reduced the available support.
Signs You May Need Bone Grafting for Dental Implants
A CBCT scan or dental X-ray may show that the implant site lacks enough bone volume. In many cases, this is when bone grafting for dental implants may be recommended to rebuild support before implant placement. The jawbone may be too narrow for standard implant placement or too short to avoid nearby anatomy.
A history of periodontal disease, long-term missing teeth, denture wear, or implant failure can also raise concern. These factors often point to reduced bone density or past bone loss.
In the lower jaw, the inferior alveolar nerve must be protected during treatment. In the upper back jaw, the maxillary sinus can limit available bone and make grafting more likely.
Situations Where Grafting Is Often Recommended
After extraction, socket preservation may be advised to help maintain the extraction socket for future implants. Ridge preservation is especially useful when the outer bone wall is thin and likely to shrink during healing.
In the upper back jaw, a sinus lift or sinus augmentation is often recommended when the maxillary sinus sits too close to the planned implant site. This is common because the upper back jaw often has limited bone height after tooth loss.
Severe ridge shrinkage may require ridge augmentation or guided bone regeneration before implant placement. In these cases, skipping grafting can compromise implant stability, esthetic outcome, and long-term functional support.
How Dentists Determine Whether You Need Bone Grafting
The evaluation starts with a full oral exam and a review of your medical history and dental history. A dentist or specialist also looks at gum health, bite forces, past extractions, and how long the tooth has been missing.
Digital imaging is a major part of the process. It helps the clinician measure available bone and identify risks before surgery. These measurements help determine whether bone grafting for dental implants may be necessary to create a stable foundation for implant placement.
Dentists should individualize the recommendation. Bone grafting is not automatic for every implant patient, and a good treatment plan explains clearly why it is or is not needed.
Imaging and Measurements
A CBCT scan gives a three-dimensional view of the implant site. It allows the dentist, periodontist, or oral surgeon to measure bone height, bone width, and bone volume while checking the position of the maxillary sinus or inferior alveolar nerve.
A dental X-ray may also be used, though CBCT is often more precise for implant planning. These images help determine implant size, angulation, and whether same-day implant placement is possible.
The restoration plan matters too. A front tooth with high esthetic demands may need more bone support than a less visible area, even if both can technically hold an implant.
Questions Patients Should Ask
Ask how much bone is missing and whether the graft serves a functional purpose, an esthetic purpose, or both. That question helps you understand whether the recommendation truly improves function or mainly improves the final appearance when bone grafting for dental implants becomes part of your treatment plan.
Ask whether the dentist can place the implant at the same visit or whether you need healing time first. You should also ask who will perform the procedure and whether a dentist, periodontist, or oral surgeon would be the best fit for your case.
For more background on bone changes after tooth loss, this resource on dental implants bone loss can help. If you are comparing broader treatment topics, the houston dental blog offers additional patient education.
Types of Bone Grafts, Healing Time, and What to Expect
Bone grafting in implant dentistry can use different graft material types and different surgical techniques. The right option depends on how much bone is missing, where the site is located, and whether implant placement will happen immediately or later.
Healing time varies widely. A small socket preservation procedure may heal faster than a large ridge augmentation or sinus lift.
Common Graft Types
An autograft uses your own bone, usually taken from another area of the mouth or body. It contains living bone components, but it also requires a donor site.
An allograft uses donor human bone that manufacturers process for safety. A xenograft comes from an animal source, commonly bovine, and an alloplast serves as a synthetic graft material that supports bone formation.
Common procedures include socket preservation after extraction, ridge augmentation to rebuild a narrow ridge, guided bone regeneration using membranes, and sinus lift treatment in the upper back jaw. Dentists choose each approach to improve implant stability and create enough support for osseointegration.
Recovery and Healing Timeline
Minor grafts may heal in a few months, while larger procedures may require a longer healing time before delayed implant placement. In some cases, dentists can place a same-day implant with grafting if the site provides strong initial stability.
Most patients can expect some swelling, mild bleeding, and discomfort for several days. Recovery usually includes a soft diet, careful oral hygiene, reduced physical activity, and follow-up visits to monitor healing.
Call your provider if you develop worsening pain, persistent bleeding, fever, unusual drainage, or signs of infection. If you are concerned about recovery after implant treatment, this article on will i be in pain after getting a dental implant may be useful.
Patients who are planning extraction and replacement may also benefit from reading why would i get dental implants after a tooth extraction and why should i consider a dental implant to replace my missing tooth. Those decisions often affect whether grafting is needed and when treatment should begin.
Alternatives, Risks, and Key Takeaways for Patients
Not every patient with reduced bone automatically needs grafting. In selected cases, alternatives such as short implants, angled implants, zygomatic implants, or a different restoration plan may reduce the need for augmentation.
These options are case-specific and depend on anatomy, bite forces, esthetic goals, and safety. Avoiding a graft only makes sense if long-term support is still adequate.
Can You Get Implants Without a Bone Graft
Yes, some patients can receive dental implants without bone grafting. This is more likely when enough native bone remains or when alternative strategies can work without compromising function.
The key is not whether patients can avoid a graft at all costs. The real question is whether skipping it would increase the risk of implant failure, poor esthetic outcome, or weak support over time.
Common Mistakes to Avoid
Delaying evaluation after tooth loss is one of the biggest mistakes. The longer you wait, the more bone resorption can occur, which may turn a simple case into one that requires jaw bone grafting.
Another mistake is assuming every graft recommendation is the same. A small socket preservation procedure is very different from major ridge augmentation or sinus augmentation.
Patients also run into trouble when choosing treatment based only on speed or price. A rushed plan that ignores bone quality, anatomical limitations, or healing needs can reduce implant success.
A practical decision framework is straightforward. Your clinician should assess bone volume, bone density, site anatomy, esthetic demands, and treatment goals, then explain whether grafting improves predictability enough to justify the added procedure.
FAQs
How do I know if I need a bone graft for a dental implant?
A dentist or specialist determines this through a clinical exam and imaging, usually a CBCT scan or dental X-ray. They measure bone height, bone width, and bone density at the planned implant site.
What is the 3/2 rule for dental implants?
The term may refer to spacing and bone considerations used in implant planning, but it is not a universal rule for every case. Ask your clinician how much bone and spacing your specific implant needs.
Are dental bone grafts really necessary?
They are necessary when there is not enough healthy bone to support an implant predictably. If a patient has adequate native bone, dentists may not need bone grafting.
What percentage of dental implants require bone grafts?
The percentage varies by practice and patient population. Bone grafting is common because many patients have some bone loss after extraction, but not every implant case requires it.
A bone graft is not a routine extra step for every implant patient, but it is often an important one when the jawbone cannot reliably support treatment. The best next move is a thorough evaluation so your dentist or specialist can match the plan to your anatomy, timeline, and long-term goals.