A tooth infection can go from “just a bad toothache” to a true dental emergency faster than most people expect. When bacteria escape the tooth and move into the jaw, face, or bloodstream, the risks shift from pain to complications like facial swelling, airway compromise, and, in rare cases, sepsis.
If you are in Houston, TX and you notice swelling, fever, or difficulty swallowing, treat it like an urgent problem, not something to watch for a few more days. A spreading tooth abscess is one of the most common reasons people end up needing emergency dentistry.
Why a Tooth Infection Can Become Dangerous
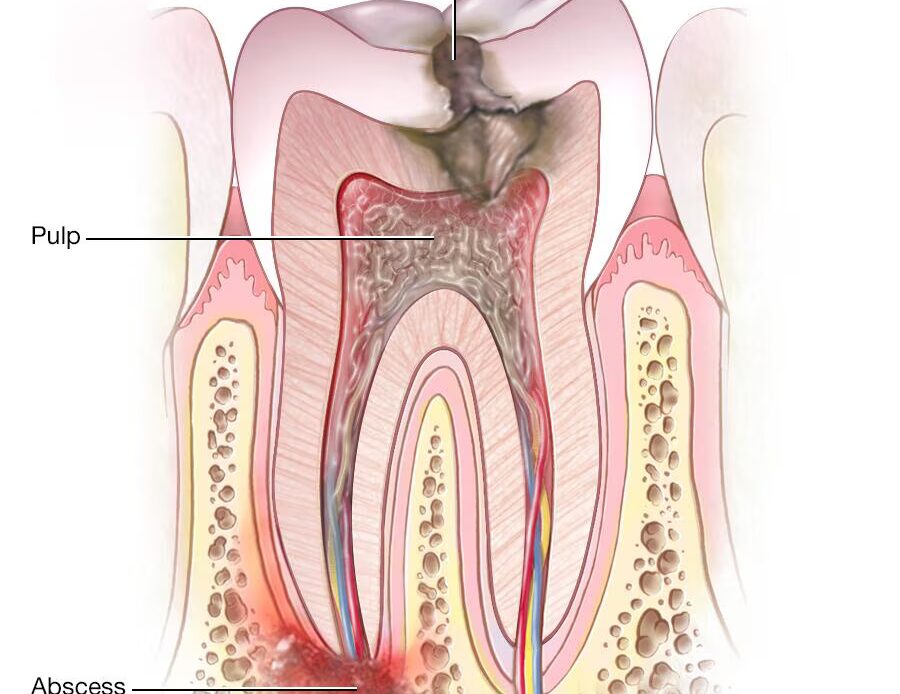
Most tooth infections start the same way: tooth decay creates a cavity, bacteria travel deeper, and the stages of tooth decay eventually reach the pulp. The pulp contains nerves and blood vessels, so once bacteria get in, pressure builds and a tooth abscess or dental abscess can form.
Trauma can do the same thing, even without a visible cavity. A cracked tooth can let bacteria reach the pulp, and a periapical abscess can develop at the root tip.
The danger comes from anatomy and pressure. The infection does not always stay trapped in the tooth, because inflammation can push bacteria and pus into the surrounding jawbone and soft tissues.
Some infections progress quickly, while others smolder for weeks. How fast it worsens depends on the tooth location, your immune response, conditions like diabetes or immunosuppression, and how long you delay treatment.
What “Spreading” Means Medically
“Spreading” has a specific meaning in healthcare, and it is not limited to pain moving around. It describes bacteria traveling beyond the tooth into nearby tissues or into the body.
Local spread includes infection moving into the gum, periodontal tissues, or jawbone. This can involve a periodontal abscess (often tied to gum disease) or bone involvement around the tooth.
Regional and systemic spread means the infection is traveling into facial spaces, lymph nodes, or the bloodstream. That is when you can see rapid jaw swelling, neck symptoms, or signs of bacteremia.
Early Warning Signs You Should Not Ignore
A spreading tooth infection usually gives early clues, even if they are easy to dismiss at first. The most common early signs are persistent toothache, pain with biting, sensitivity to hot or cold, and a bad taste from drainage.
Look closely at your gums and face. A pimple-like bump on the gum, redness, warmth, cheek swelling, or jaw swelling can mean pus is trying to escape or is building under the tissue.
System symptoms matter. Fever, fatigue, and swollen or tender lymph nodes are escalation signals, not “normal tooth pain.”
Symptoms That Suggest the Infection Is Moving Beyond the Tooth
Facial swelling that increases over hours, tenderness that spreads across the jawline, or pain that radiates toward the ear or down the neck can indicate the infection is leaving the tooth area. These patterns are common when infection tracks through soft tissue planes.
Trismus, meaning difficulty opening the mouth, is a serious warning sign. A worsening sore throat, hoarse voice, or difficulty swallowing should also raise concern for deeper spread and possible airway compromise.
How a Tooth Infection Spreads Through the Body
A tooth abscess spreads through a few predictable pathways. Bacteria can exit through the root tip into bone, travel through the spaces between muscles and connective tissues (fascial planes), or enter the blood and cause bacteremia.
Clinical research on odontogenic infections and their complications shows how untreated dental infections can spread beyond the tooth and lead to serious systemic issues.
Tooth location changes the risk profile. Lower molar infections can drop into spaces under the tongue and jaw, which is why they can threaten breathing, while upper tooth infections can push into the maxillary sinus and cause sinus involvement.
Antibiotics can reduce bacterial load, but they often cannot eliminate the source if the tooth remains infected. If the pulp is necrotic or there is a walled-off abscess, you usually need source control with root canal treatment, incision and drainage, or tooth extraction.
Common Routes of Spread
Periapical spread starts at the root tip, often from a periapical abscess, and moves into the alveolar bone and surrounding soft tissues. This can lead to cellulitis, where infection spreads diffusely through tissue rather than staying in a contained pocket.
Hematogenous spread happens when bacteria enter the bloodstream. Most healthy people clear transient bacteremia, but in rare cases it can progress to sepsis, especially when treatment is delayed or immunity is compromised.
Who Is at Higher Risk in Houston
Certain health factors make spread more likely and recovery slower. Diabetes, immunosuppression, and pregnancy can change how your body responds to bacteria and inflammation.
Life factors matter too, especially in a large city where people may delay care. Smoking, advanced gum disease, and avoiding treatment due to cost or fear can allow an infection to grow until it becomes a dental emergency.
If you are unsure whether you are dealing with a tooth problem or a gum problem, it helps to understand the differences between infections that start in the tooth versus the gums. This breakdown on how dentists tell tooth-origin pain from gum-origin infections can clarify why treatment plans differ:
Potential Complications If the Infection Keeps Spreading
Local complications are common and still serious. These include cellulitis, osteomyelitis (bone infection), sinus involvement, tooth loss, and worsening periodontal breakdown.
Deep-space infections are less common but far more dangerous. Ludwig’s angina, a rapidly spreading infection in the floor of the mouth, can cause neck swelling and airway compromise and requires immediate emergency care.
Systemic complications are the red-line scenario. In these cases, sepsis can occur, and some patients with certain heart conditions may face endocarditis risk when bacteria circulate in the bloodstream.
Sepsis: The Red-Flag Scenario
Sepsis is a body-wide inflammatory response to infection, and it can escalate quickly. Warning signs include high fever, chills, rapid heart rate, confusion, extreme weakness, and low blood pressure.
If these symptoms appear with a suspected dental abscess, call 911 or go to a Houston-area ER immediately. Do not try to “sleep it off” or wait for a dental appointment the next day.
Can It Spread to the Brain?
It is rare, but yes, severe complications can involve the brain. Dental and facial infections can spread through venous pathways and lead to cavernous sinus thrombosis, or, less commonly, a brain abscess.
Urgent symptoms include severe headache, swelling around the eyes, vision changes, drooping eyelid, confusion, or other neurologic symptoms. These require emergency evaluation, even if the tooth pain itself is not severe.
What to Do Right Away in Houston (Step-by-Step)
Start with urgency based on symptoms, not just pain level. If you have facial swelling, jaw swelling, fever, drainage with a bad taste, or severe pain, call an emergency dentist for a same-day evaluation.
If breathing or swallowing is affected, swelling is rapidly increasing, or you have systemic symptoms, go straight to the ER. Airway risk and suspected sepsis are hospital problems first, dental problems second.
Avoid “wait and see.” Write down when symptoms started, whether swelling is growing, your temperature, and what medications you have taken, because that timeline helps triage and treatment decisions.
If you are looking for a place that offers urgent dental evaluation, Dr. Friedberg and Associates provides same-day help through their emergency dental care services when appropriate:
Safe At-Home Measures While You Arrange Care
Use over-the-counter pain relievers as directed on the label, unless your physician has told you to avoid them. A cold compress on the cheek can help with swelling and pain management.
Do not apply heat to the face, because it can increase blood flow and worsen swelling. Do not attempt to drain the abscess yourself, and do not poke the gum bump, since that can push bacteria deeper.
Where People Commonly Seek Care in Houston
Emergency dental clinics can evaluate the tooth, take dental X-rays, and provide treatment such as incision and drainage when appropriate. They can also determine whether root canal treatment or infected tooth extraction is the safest next step.
Hospital ERs are appropriate when there is airway risk, severe facial swelling, dehydration from inability to swallow, uncontrolled pain, or suspected sepsis. ER teams can stabilize you and coordinate imaging like CT when deep-space infection is a concern.
How Dentists Treat a Spreading Tooth Infection
Treatment starts with diagnosis and risk assessment. Dentists use an exam, percussion testing, temperature testing, dental X-rays, and sometimes a CT referral if they suspect deep-space involvement.
The core principle is source control. That means removing the infection source with root canal treatment, incision and drainage, or tooth extraction, rather than relying on antibiotics alone.
Dentists prescribe antibiotics when needed, especially for fever, cellulitis, rapidly spreading swelling, or patients with higher immune risk. They also manage pain alongside treatment and create a clear follow-up plan to confirm the infection resolves.
Root Canal vs. Extraction: How the Decision Is Made
A root canal is preferred when the tooth is restorable and the canals can be cleaned, disinfected, and sealed. This removes infected pulp tissue and keeps the natural tooth in place.
Tooth extraction is recommended when the tooth is non-restorable, a fracture is present, or infection persists despite appropriate care. In some cases, an infected tooth extraction is the safest way to eliminate the source quickly.
If you lose a tooth, planning the replacement matters for bite stability and bone health. These pages explain options people often consider after removal, including whether a dental implant is a smart replacement and why some patients choose implants after an extraction.
What Happens After Treatment
Most people start to feel meaningful improvement within 24 to 72 hours after dentists control the source, although swelling may take longer to fully resolve. If your dentist prescribes antibiotics, you should finish the full course, even if symptoms improve early.
Seek re-evaluation if you develop new or worsening swelling, fever, increasing pain, foul drainage, or trouble swallowing. Those can signal persistent infection, inadequate drainage, or a deeper-space problem.
Common Mistakes That Make Tooth Infections Worse
The biggest mistake is relying on antibiotics alone without treating the infected tooth. Antibiotics may temporarily reduce symptoms, but the infection often returns if the source remains.
Delaying care after swelling starts is another common issue, especially if pain comes and goes. Using leftover antibiotics is risky because the drug may be wrong for the bacteria, the dose may be inadequate, and it can delay proper treatment.
Ignoring risk factors slows healing. Poor diabetes control, smoking, unmanaged gum disease, and inconsistent oral hygiene can all increase recurrence risk and prolong inflammation.
If your infection is tied to gum disease, address the foundation problem too. This overview of how gum disease can lead to tooth loss explains why periodontal health affects long-term outcomes:
If the tooth feels loose, do not assume it will “tighten up” on its own. A loose tooth in adults can signal advanced infection or bone loss that needs prompt evaluation: https://drfriedbergandassociates.com/loose-tooth-in-adults/
Myths to Correct
Pain stopping does not mean the infection is gone. Sometimes the nerve dies, reducing pain while bacteria continue spreading through bone and soft tissue.
“Popping” a gum boil is not a fix. It can drive bacteria deeper, worsen cellulitis risk, and delay the incision and drainage or definitive dental treatment you actually need.
Prevention and When to Schedule Follow-Up in Houston
Prevention starts with controlling tooth decay and gum disease. Brush with fluoride toothpaste, keep up with flossing, and limit sugary drinks and frequent snacking, since repeated sugar exposure fuels cavities.
Routine dental exam visits and a professional dental cleaning catch problems before the pulp gets involved. Early cavities are easier to treat, and you avoid the cascade that leads to a periapical abscess.
After an abscess, schedule definitive care and restoration, such as a crown or filling after root canal treatment, to prevent reinfection. If extraction was necessary, talk about replacement options early so shifting teeth and bone loss do not create a second problem.
Houston-Specific Practical Tips
Know your nearest 24/7 hospital and have an emergency dental option saved for nights and weekends. When swelling or fever appears, hours matter more than convenience.
If you live in flood-prone areas, keep dental records and insurance information accessible on your phone. After major disruptions, prioritize urgent swelling, fever, and difficulty swallowing, because delays tend to compound quickly.
FAQ
What is the 3 3 3 rule for tooth infection?
The “3 3 3 rule” is a rule of thumb some people use to gauge urgency, such as symptoms worsening over hours to days. It is not a medical standard, and swelling, fever, facial redness/warmth, or difficulty swallowing should be treated as same-day problems.
What do they do if a tooth infection has spread?
Dentists focus on source control: root canal, incision and drainage, or tooth extraction, depending on the tooth’s condition and where the infection is tracking. Antibiotics may be prescribed when there is fever, cellulitis, spreading swelling, or higher medical risk, and the ER is appropriate for airway concerns or suspected sepsis.
What are the first signs of sepsis from a tooth abscess?
High fever, chills, rapid heart rate, confusion, extreme weakness, and low blood pressure are major warning signs. If these occur with a suspected dental abscess, seek emergency care immediately.
How fast can a tooth infection spread to your brain?
It is uncommon, but serious complications can develop quickly if infection spreads through facial spaces or blood vessels. Severe headache, eye swelling, vision changes, or neurologic symptoms should be treated as an emergency, even if the tooth pain seems manageable.