A dental infection can start with one sore tooth or a strip of irritated gums, but the next steps are not the same. Knowing whether the problem is more likely a tooth infection or a gum infection can help Houston, TX patients get the right care faster and avoid a small issue turning into a dental abscess.
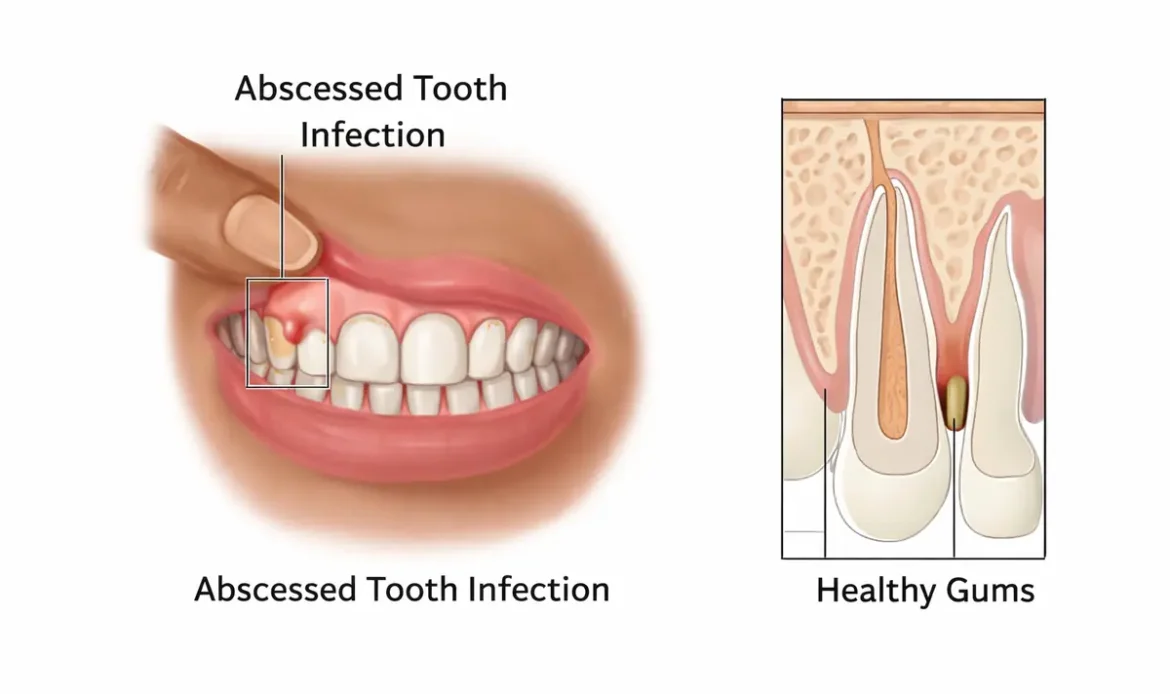
What Makes Tooth and Gum Infections Different
A tooth infection usually starts inside the tooth or around its root. It is often linked to tooth decay, a deep cavity, trauma, a cracked tooth, or a failed filling that allows bacteria to reach the pulp.
A gum infection starts in the soft tissues around the teeth. It is commonly tied to plaque, tartar, gingivitis, periodontitis, and other forms of gum disease or periodontal disease.
When comparing a tooth vs gum infection, both can cause pain, swelling, and a foul taste. The main difference is where the infection begins, how it spreads, and what treatment will actually stop it.
Where a Tooth Infection Starts
Most tooth infections begin in the pulp, root, or near the tooth apex. That is why a pulp infection often causes deep internal pain rather than surface soreness.
Common triggers include untreated tooth decay, a large cavity, a cracked tooth, or a failed filling. Once bacteria enter the inner tooth, pressure can build quickly and lead to a tooth abscess.
Where a Gum Infection Starts
A gum infection usually begins at the gumline or inside a periodontal pocket around the tooth. This often happens when plaque and tartar stay below the gums long enough to trigger inflammation.
Early cases may start as gingivitis. More advanced infection can move into periodontitis, where the supporting tissues and bone are affected.
Symptoms That Point to a Tooth Infection
A tooth infection usually causes pain that feels focused and intense. Patients often describe sharp pain, throbbing pain, or persistent pain centered on one tooth.
Tooth sensitivity is another strong clue. Hot sensitivity, cold sensitivity, and pressure when chewing are common when the root or pulp is involved.
Some people say the tooth feels taller then the others. Others notice chewing sensitivity, pressure sensitivity, or a tooth that hurts when tapped.
If you want, I can give you one more perfectly placed external link for the tooth infection side so the article is fully balanced.
Common Tooth Infection Warning Signs
Watch for these signs when a tooth infection is more likely:
- Persistent toothache that does not fade
- Sharp pain or throbbing pain in one tooth
- Swelling in the cheek or jaw near one tooth
- Pressure when chewing or biting
- Hot sensitivity or cold sensitivity
- Jaw pain that seems tied to one area
- A pimple-like bump on the gum near one root
Signs the Infection May Be Spreading
A spreading tooth abscess can cause facial swelling, cheek swelling, fever, swollen lymph nodes, pus drainage, and a bad taste or foul taste in the mouth. At that stage, the issue is no longer just a simple toothache and may be part of a more serious tooth vs gum infection.
Trouble opening the mouth, difficulty swallowing, or difficulty breathing needs urgent care right away. Those symptoms can signal a serious dental infection that requires immediate attention, especially when a tooth vs gum infection is spreading.
Symptoms That Point to a Gum Infection
A gum infection usually feels less isolated. Instead of one tooth causing trouble, the gums may feel sore, puffy, and tender across several teeth.
Red gums, swollen gums, bleeding gums, and gum tenderness are common early signs. Bad breath, gum recession, and changes in your gums or breath often point to an underlying periodontal problem rather than a single infected tooth.
Pain may feel more like a dull ache or diffuse soreness. Some patients only notice discomfort when brushing, flossing, or eating crunchy foods.
Common Gum Infection Warning Signs
These symptoms often lean toward a gum infection:
- Bleeding gums when brushing or flossing
- Swollen gums or red gums along the gumline
- Gum tenderness in more than one area
- Bad breath that keeps returning
- A dull ache rather than one sharp point of pain
- Gum recession or teeth that look longer
- Soreness around several teeth at once
When Gum Disease Becomes More Serious
Advanced gum disease can create deep periodontal pockets, pus near the gums, and teeth that feel loose. In some cases, a periodontal abscess forms and causes localized swelling with drainage.
Untreated periodontitis can lead to bone loss and reduced tooth support. If you have teeth that feel loose as an adult, the problem may involve infection in the gums and supporting structures rather than the tooth alone.
Tooth Infection vs Gum Infection: Side-by-Side Comparison
A quick comparison helps when symptoms overlap. Both conditions can become a dental abscess, and both deserve prompt evaluation.
| Comparison point | Tooth infection | Gum infection |
|---|---|---|
| Pain type | Sharp pain, throbbing pain, disruptive pain | Dull ache, soreness, tenderness |
| Pain location | Usually one tooth | Often spread along the gums |
| Chewing sensitivity | Common, especially pressure when chewing | May occur, but less focused on one tooth |
| Temperature sensitivity | Hot sensitivity and cold sensitivity are common | Less common |
| Gum bleeding | Not always present | Common |
| Bad breath | Can happen with pus drainage | Common, especially with periodontal disease |
| Visible swelling | Near one tooth, cheek swelling, jaw swelling | Along the gumline or in a periodontal pocket |
| Pus | Often from a tooth abscess | May occur with a periodontal abscess |
| Fever | More likely if infection spreads | Possible in advanced infection |
| Likely cause | Cavity, pulp infection, cracked tooth, failed filling | Plaque, tartar, gingivitis, periodontitis |
| Typical treatment | Root canal therapy, drainage, antibiotics, or removal | Deep cleaning, scaling and root planing, periodontal care |
Best Comparison Points to Include
If the pain is intense, one-sided, and triggered by biting or temperature, a tooth infection is more likely. If the gums are bleeding, swollen, and tender in several areas, a gum infection is more likely.
A tooth infection is often isolated at first. A gum infection often affects a wider area because the bacteria spread along the gumline and below it.
How Houston Patients Can Tell the Difference at Home
Start with the location of the pain. If one tooth hurts when you bite down or reacts strongly to heat and cold, that points more toward a tooth infection.
If your gums are bleeding, swollen, sore in more than one area, or you have chronic bad breath, the problem may be gum-related. Many patients with periodontal disease first notice changes in their gums or breath before they feel severe pain.
Questions to Ask Yourself
Ask yourself these questions:
- Does one tooth hurt when you bite down?
- Do you have hot sensitivity or cold sensitivity in one tooth?
- Are your gums bleeding, swollen, or receding in several spots?
- Is the pain more of a toothache or more of a sore gumline?
- Do you notice pus drainage, a foul taste, or swelling near one root?
What Not to Do
Do not rely on home remedies if swelling is getting worse or the pain is severe. Salt water rinses may soothe tissue, but they do not remove infected pulp or clean a deep periodontal pocket.
Do not ignore symptoms just because they come and go. Some infections drain temporarily, which can reduce pressure for a short time while the underlying problem keeps spreading.
When to Seek Urgent Dental Care in Houston
Both conditions can worsen quickly. Waiting too long increases the risk of a larger dental abscess, more swelling, missed work, and more complex treatment, especially when you leave a tooth vs gum infection untreated.
Urgent warning signs include fever, facial swelling, pus drainage, foul taste, and difficulty swallowing. If symptoms spike overnight or on a weekend, same-day dental care from an emergency dentist matters when a tooth vs gum infection becomes severe.
Emergency Red Flags
Get urgent help for:
- Rapid swelling
- Severe throbbing pain
- Visible abscess
- Fever
- Swollen lymph nodes
- Difficulty swallowing
- Difficulty breathing
Difficulty breathing or swallowing requires emergency medical attention immediately. Those symptoms should never be watched at home.
Houston Access Considerations
Patients in Downtown Houston, The Heights, Memorial, Katy, Sugar Land, and Cypress often need local care that is easy to reach fast. Prompt treatment can prevent a smaller infection from becoming a more painful and expensive problem.
How Dentists Diagnose and Treat Each Condition
Diagnosis usually starts with an oral exam and dental X-rays when evaluating a tooth vs gum infection. Dentists also look for swelling, drainage, gum depth changes, pressure sensitivity, and signs of bone loss.
Treatment depends on where the infection started. In a tooth vs gum infection, a tooth-root problem and a periodontal problem may look similar from the outside, but they are treated very differently.
Typical Treatment for a Tooth Infection
A tooth infection often needs root canal treatment to remove infected tissue from inside the tooth. Root canal therapy addresses the source rather than just masking pain.
Antibiotics may be used when swelling, fever, or spreading infection is present, but antibiotics alone are not always enough. If the tooth cannot be saved, surgical removal of the damaged tooth may be necessary.
If extraction is required, many patients later ask about options for replacing a missing tooth with an implant. Others want to know why implants are often considered after removal.
Typical Treatment for a Gum Infection
A gum infection is treated by removing plaque, tartar, and bacteria from below the gumline. That often means deep cleaning, scaling and root planing, drainage when needed, and a personalized periodontal care plan.
The goal is to reduce inflammation, shrink pocket depth, and protect bone and tooth support. If infection has already affected stability, you can read more about how advanced gum problems can lead to tooth loss.
Which Problem Is More Likely Based on Your Symptoms
Use the symptom pattern as a clue, not a diagnosis. A dentist still needs to confirm the source with an exam and imaging.
More Likely a Tooth Infection If
- One tooth has severe pressure sensitivity
- Heat or cold triggers sharp pain
- You feel a focused toothache on one side
- There is swelling near one root area
- You see a bump on the gum near one tooth
- The pain feels deep and disruptive
More Likely a Gum Infection If
- Several teeth seem affected because the gums are inflamed
- You have bleeding gums and swollen gums
- Bad breath has been building over time
- Gum recession is becoming more noticeable
- Teeth that feel loose are part of the problem
- The soreness follows the gumline rather than one tooth
Prevention Tips for Houston Families
Most infections start with problems that were preventable. Daily care and regular checkups reduce the risk of both tooth infection and gum infection.
Brushing twice daily with fluoride toothpaste and flossing every day help limit plaque and bacteria. Routine cleanings also catch small cavities, early gingivitis, and early periodontitis before they turn into painful emergencies.
Habits That Lower Risk
- Brush twice daily with fluoride toothpaste
- Floss daily
- Keep regular exams and cleanings
- Treat a cavity early before it reaches the pulp
- Address bleeding gums before inflammation gets worse
- Stay consistent with periodontal maintenance if you have past gum disease
- Tell your dentist about dry mouth, diabetes, or smoking history
FAQ
How Do You Tell If You Have a Gum or Tooth Infection?
A tooth infection usually causes deep, focused pain in one tooth, often with pressure sensitivity or temperature sensitivity. A gum infection more often causes red gums, swollen gums, bleeding gums, bad breath, and soreness along the gumline.
What Is the 3-3-3 Rule for Tooth Infection?
You may see the so-called 3-3-3 rule online, but it is not a formal dental standard. If you suspect an infection and notice swelling, fever, worsening pain, or drainage, contact a dentist right away for evaluation.
What Is a Stage 4 Gum Infection?
People often use that phrase to describe advanced periodontal disease. It may involve deep infection, gum recession, bone loss, loose teeth, and a high need for professional periodontal care.
How Do You Know If It’s a Toothache or Gum Pain?
A toothache usually centers in one tooth and often worsens with biting, heat, or cold. In contrast, gum pain feels sore, swollen, or tender across the gums and may include bleeding or bad breath.