Periodontal treatment is less mysterious than most people think. It usually starts with tiny measurements around each tooth and ends with a plan to stop gum disease from quietly damaging bone.
The goal is control, not perfection, because periodontal disease behaves more like a chronic bacterial infection than a one-time cavity fix.
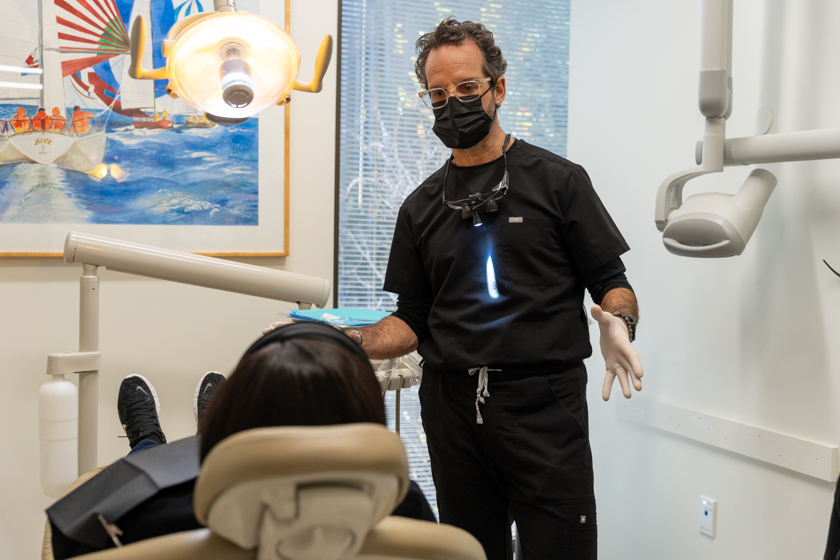
Why Periodontal Treatment Is Done
Periodontal disease begins as a bacterial infection driven by plaque biofilm and subgingival calculus that triggers inflammation in the gums. Early on, gingivitis develops, causing red, puffy gums that bleed easily but typically without bone loss.
When gingivitis progresses to periodontitis, the condition moves deeper. The American Academy of Periodontology explains how untreated periodontal disease can lead to attachment loss and bone destruction over time.
The attachment between the tooth and gum breaks down, periodontal pockets form. Consecutively, clinical attachment loss and bone loss develop if you do not control the infection.
Subgingival calculus, tartar, and biofilm trapped inside periodontal pockets accelerate destruction when clinicians do not remove them through scaling and root planing.
Treatment goals are straightforward: reduce bacterial infection, shrink periodontal pockets, control inflammation, and protect the bone and gum tissue that hold teeth in place.
A good outcome often looks like less bleeding on probing, shallower pocket depth readings, reduced halitosis, and stable tooth mobility rather than “perfect” gums overnight.
Care can be provided by a general dentist, a dental hygienist, or a periodontist depending on severity. Referral to a periodontist is common when pockets are deep, bone loss is visible on radiographs, recession is significant, pus is present, or prior nonsurgical treatment did not hold.
Signs You Might Need Periodontal Care
Bleeding gums that happen during brushing technique or flossing are one of the earliest clues. Swelling, persistent halitosis (bad breath), gum recession, pus at the gumline, loose teeth, tooth sensitivity, and bite changes are stronger warning signs that periodontitis may be present.
Risk factors matter because they change how aggressively gum disease progresses. Smoking, diabetes, genetics, certain medications that affect saliva or gum tissue, and inconsistent oral hygiene — including not using interdental brushes — all raise the odds that inflammation turns into lasting clinical attachment loss and bone damage.
Step 1: The Periodontal Evaluation and Diagnosis
The first appointment is an initial assessment that looks at more than just your teeth. Expect a review of medical history, dental history, current symptoms, medications, smoking status, and conditions like diabetes that can affect healing and inflammation.
Next, the clinician examines the gums and supporting tissues. They perform periodontal charting using periodontal probing to measure pocket depth around each tooth, usually at multiple points per tooth.
The clinician takes or reviews dental X-rays to evaluate bone levels and detect tartar or subgingival calculus that may not be visible above the gumline. By combining probing and imaging, the provider separates simple gingivitis from periodontitis with attachment loss and bone loss.
What the Measurements Mean
Pocket depth is a practical marker of inflammation and attachment changes. Deeper readings often mean the gum has detached from the tooth and the pocket is harboring bacteria, plaque biofilm, and subgingival calculus.
Bleeding on probing signals active inflammation. In addition, clinicians evaluate plaque levels, calculus accumulation, gum recession, tooth mobility, and radiographs to determine how intensive periodontal treatment should be.
Your Personalized Treatment Plan
Treatment usually begins with a nonsurgical approach and progresses to surgical options if needed. Factors such as pocket depth, bone loss patterns, furcation involvement (bone loss between roots), clinical attachment loss, and your response to deep cleaning all influence that decision.
You should also get clarity on numbing options such as local anesthetic, number of visits, recall interval recommendations, and what “success” means for your case.
Many offices will discuss expected outcomes in plain terms, similar to guidance you may see from patient education sources like Cleveland Clinic and Mayo Clinic, while tailoring it to your measurements and risk factors.
Adjunct therapies may include antimicrobial mouthwash, chlorhexidine rinses, localized antibiotics placed into periodontal pockets, or subgingival irrigation when bacterial infection is more advanced.
Step 2: Nonsurgical Periodontal Treatment (Deep Cleaning)
Deep cleaning is the common name for scaling and root planing. Scaling removes plaque and tartar above and below the gumline, including hardened subgingival calculus that keeps the infection active.
Root planing smooths the root surfaces so the gums can heal and tighten against the tooth. Smoother roots also make it harder for biofilm to stick and easier for you to maintain oral hygiene at home.
What Happens During Scaling and Root Planing
Most patients receive a local anesthetic so the appointment feels like pressure and vibration rather than pain. Clinicians often divide treatment into quadrant scaling, treating one side or one quarter of the mouth per visit.
Your clinician may use an ultrasonic scaler to break up calculus with vibration and water flow. They then use hand instruments to fine-scale and remove subgingival calculus along the root surface.e-scale and remove subgingival calculus along the root surface.
When deeper periodontal pockets persist, the clinician may recommend localized antibiotics, antimicrobial mouthwash, chlorhexidine, or subgingival irrigation to reduce bacterial infection
How Long It Takes and What It Feels Like
Appointment time depends on how many teeth are treated and how heavy the calculus buildup is under the gums. Many visits run about 45 to 90 minutes, and it is common to need one to several visits if multiple quadrants require care.
Afterward, mild tooth sensitivity, post-treatment bleeding, tenderness, and temporary inflammation can occur for 24 to 48 hours. Over-the-counter pain relievers, gentle brushing technique, warm saltwater rinses, and sometimes antimicrobial mouthwash usually handle it, but severe pain, swelling, or pus warrants a call.
Step 3: When Surgery or Advanced Procedures Are Needed
Clinicians consider surgery when deep periodontal pockets persist after nonsurgical treatment or when bone loss becomes advanced. The goal is to reduce pocket depth so you can clean more effectively and keep the tissues stable long term.
During flap surgery, also called pocket reduction surgery, the clinician gently lifts the gum tissue to remove deep calculus and infected tissue, then repositions the gums to improve access and make home care easier.
The clinician may place sutures and remove them at follow-up visits, where they use periodontal probing and radiographs to re-check healing and attachment levels.
Common Surgical and Regenerative Options
Regenerative procedures may be recommended in select cases where rebuilding support is realistic. Bone grafting and guided tissue regeneration can help restore some lost support around teeth. Especially in certain defect shapes seen on dental X-rays.
Soft tissue graft options can address gum recession and root exposure. If you are exploring cosmetic and comfort-focused solutions for recession, you can read about procedures offered through our periodontal plastic surgery services.
If teeth show increased tooth mobility, clinicians can sometimes use splinting to stabilize them during healing. When severe clinical attachment loss and bone loss create a poor prognosis, the provider may recommend extraction before discussing dental implants.
Aftercare, Maintenance, and What Results to Expect
The first week after periodontal treatment is about protecting healing tissue while keeping bacterial infection under control. Many patients do best with softer foods for a day or two. Careful brushing technique near tender areas, modified flossing, and warm saltwater rinses.
Pain control is usually simple, but follow your clinician’s instructions if they prescribe antibiotics, antimicrobial mouthwash, or chlorhexidine. If local anesthetic numbed the area, avoid chewing until sensation returns.
Long-term success depends on periodontal maintenance cleaning appointments that are more frequent than a standard six-month recall interval.
If you are specifically looking for local scheduling details and what a more frequent recall program looks like, our Houston periodontal maintenance information is here.
Clinicians usually measure success by checking for reduced bleeding on probing, healthier tissue color and firmness, shallower periodontal pockets. Stable radiographs showing no further bone loss, reduced halitosis, and stable tooth mobility.
Common Mistakes That Slow Healing
Skipping periodontal maintenance visits is the fastest way to relapse, even after excellent deep cleaning or surgery. Periodontitis can re-activate when plaque biofilm and subgingival calculus rebuild in periodontal pockets.
Smoking slows healing and increases recurrence risk. Inconsistent oral hygiene, rushing flossing, not using interdental brushes, or stopping antimicrobial mouthwash too early can keep inflammation active.
Do not ignore ongoing symptoms like persistent bleeding, swelling, pus, halitosis, or loose teeth. Those are signals to re-check pocket depth, radiographs, bite forces, and whether additional therapy is needed.
Mini Case Examples (What Patients Commonly Experience)
Mild-to-moderate periodontitis often responds well to scaling and root planing plus improved brushing technique and tighter recall interval scheduling.
A typical pattern is less bleeding within weeks, improved pocket depth readings at re-evaluation, and stability with regular periodontal maintenance cleanings.
Advanced periodontitis often needs a staged approach: deep cleaning first, then flap surgery, regenerative procedures, or splinting in areas that do not respond.
Long-term control usually requires strict maintenance, diabetes management, smoking cessation, consistent use of interdental brushes, and periodic dental X-rays to monitor bone levels.
FAQ
How Painful Is Periodontal Treatment?
Most patients report pressure more than pain because local anesthetic is commonly used for scaling and root planing. Soreness, tooth sensitivity, and minor post-treatment bleeding for 1 to 2 days is common.
What Do They Do at a Periodontal Appointment?
A periodontal visit usually includes an examination, periodontal charting with periodontal probing, evaluation of pocket depth, review of radiographs, and assessment of gum recession. Depending on the visit, scaling, root planing, or periodontal maintenance cleaning may also be performed.
How Long Does a Periodontal Deep Cleaning Take?
Timing depends on severity and whether care is split into quadrant scaling. Many patients need one to several visits, and each visit is often around an hour. Sometimes longer when subgingival calculus buildup is significant.
Do They Numb You for Periodontal Cleaning?
Yes, deep cleaning is frequently done with local anesthetic to keep you comfortable, especially when pocket depth readings are higher or inflammation is active. If you are anxious or sensitive, discuss numbing options before treatment begins.